Sinusitis: Causes, Types of Sinusitis, Diagnosis, Treatment
Jul 24, 2023

Inflammation or swelling of the tissue lining your sinuses is known as sinusitis. Structures inside your face called sinuses are usually air-filled. Allergies, viral infections, and bacterial infections can aggravate them to the point where they become clogged and fluid-filled. In addition to other symptoms including a stuffy nose and facial pain and pressure, this can also induce nasal congestion. Another name for sinusitis is rhinosinusitis.

Etiology of Acute Sinusitis
- Nasal Infection: Most acute sinusitis start as viral infections followed by bacterial invasion
- Swimming and diving
- Trauma
- Dental infection- Predisposing factors for maxillary sinus can be due to dental infection. Maxillary sinus is related to the 2nd premolar and 1st molar.
Also Read: Tinnitus: Causes, Symptoms, Risk Factors, Diagnosis, Treatment, Prevention and Complications
Causes of Acute Sinusitis
All the sinus have their own drainage pathway or drainage ostia. If there is obstruction to the ventilation of the sinuses due to edema, mucus, polyps, URTI hence there will be inflammation of all the mucosal lining of sinuses. These inflammation of mucosal cells produce exudate which can be sterile or infected. If sinus is infected it is known as Suppurative sinusitis. If non-infected known as Sterile sinusitis. Majority of cases, bacterial infection occurs. Most common bacteria for causing acute sinusitis: S.pneumoniae. Sinusitis of dental origin, the bacteria affected is Mixed infection (aerobic and anaerobic infection).
Also Read: Disorders of the voice: Causes, Symptoms, Risk Factors, Diagnosis and Treatment
Predisposing Factors of Acute Sinusitis
- Obstruction to sinus ventilation and drainage
- Stasis of secretion in nasal cavity (cystic fibrosis) - Ciliary motility defect predispose to mostly chronic sinus infection
- Allergy- Mucosal edema will obstruct the ventilation of sinuses causing retention of secretion and infection resulting in sinusitis
Systemic factors
- Attack of exanthematous fever (measles, chicken pox, whooping cough)
- Nutritional deficiencies
- Immune deficiencies
Bacteriology
Bacteria such as Streptococcus pneumoniae, H.influenza, Moraxella, Streptococcus pyogenes, Staphylococcus aureus results in acute sinusitis, Anaerobic organisms and mixed infections are seen in sinusitis of dental origin.
Sinusitis Secondary to Dental Infection
- Secondary to infections of roots of molar and 2nd premolar teeth
- Causes maxillary sinusitis
- Oroantral fistula following tooth extraction is a cause
- Oroantral fistula is communication between maxillary sinus and oral cavity
- Anaerobic organisms and mixed infections are seen in sinusitis of dental origin
- Dental infections are very fulminating and result in suppurative sinusitis
Also Read: Aeroplane Ear: Causes, Symptoms, Risk Factors, Diagnosis, Treatment, Prevention and Complications
Clinical features of Acute Sinusitis
Major criteria Minor criteria Nasal obstruction
Facial pain or pressureHeadache Purulent nasal discharge Cough Fever Halitosis Nasal congestion Ear pain and pressure Hyposmia or anosmia Dental pain Facial congestion or fullness NA
For diagnosis 2 major or 1 major and 2 minor symptoms are required:
| Maxillary | Frontal | Ethmoid | Sphenoid | |
| Headache or pain | Usually seen over cheek and forehead and can be confused with frontal sinusitis | Localised to frontal sinuses above medial canthus | Localised over bridge of nose, medial and deep to the eye | Occiput or vertex |
| Tenderness | Cheek (pressing over canine fossa) | Over frontal sinus (pressing on the floor of frontal sinus) | Bridge of nose | NIL |
| Redness and edema | Cheek, lower eyelid swelling | Upper eyelid puffiness | Both eyelids become puffy | NIL |
| Site of nasal discharge | Middle meatus | Vertical streak of mucopus high up in anterior portion of middle meatus | Seen in middle or superior meatus depending on involvement of anterior or posterior group | Seen in posterior rhinoscopy on the roof and posterior wall of nasopharynx |
| Early Complications | Orbital cellulitis, Osteomyelitis, Frontal sinusitis | Orbital cellulitis, Osteomyelitis, intracranial abscess | Orbital cellulitis, vision loss, cavernous sinus thrombosis, intracranial abscess |
- Pus in sphenoethmoidal recess leads to sphenoid sinusitis
- Pus in superior meatus leads to posterior ethmoidal sinusitis
- Pus in middle meatus leads to Frontal or Maxillary or Anterior ethmoidal sinusitis
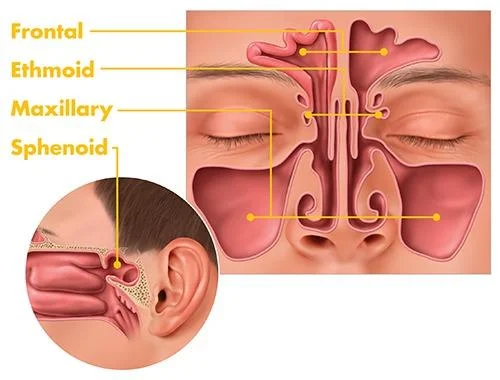
Maxillary Sinusitis
Postural test is done to differentiate maxillary sinus from frontal and ethmoidal sinusitis. Clean the pus in the middle meatus and then put the patient in head lying (tilt) opposite side. If there is reappearance of pus, then it is identified as maxillary sinusitis. If no reappearance of pus, ask the patient to sit upright head hanging down position, gravity depended reappearance of sinus indicates Frontal sinusitis. If no reappearance on both positions, then it is called Ethmoidal sinusitis.
Frontal Sinusitis
Pain has characteristic periodicity or Office headache While sleeping, anti-gravity position will cause retention of secretion in frontal sinus, the sinus with full of pus while wake-up causes severe headache in morning. In sitting position throughout the day, there will be gravity depended drainage by evening sinus become little less accumulation with no headache. Tenderness on the floor of frontal sinus just above medial canthus. Edema of upper eyelid.

Ethmoidal Sinusitis
Pain is located on the bridge of nose, deep to the eye, aggravated by movements of eyeball Orbital cellulitis.
Sphenoidal Sinusitis
Characteristic feature: Vertex headache or occipital headache and Post nasal discharge.
Also Read: Perforated Eardrum: Functions, Causes, Symptoms, Diagnosis, Treatment, Prevention and Complications
Diagnosis of Acute Sinusitis
- Clinical examination
- Diagnostic nasal endoscopy
- X-ray is the FIRST investigation to be done
- CT scan in acute sinusitis is done only when a high risk complication is anticipated
- Sinus Puncture and Bacterial Culture- Gold standard for Diagnosing Bacterial Sinus Infection
- Accurate method of diagnosis is sinuscopy and biopsy
Treatment of Acute Sinusitis
- Medical: Antibiotic TOC + decongestants + analgesics + hot fomentation
- Surgical: If no response to medical therapy,If it’s progressing to complication or FESS (most preferred) /Ethmoidectomy/Trephination of frontal sinus
Chronic Sinusitis
Failure of resolution of acute infection for more than 12 weeks . Maxillary sinus is most commonly involved. Symptoms include Purulent nasal discharge is the most common symptom with nasal obstruction. Syndromic causes and ciliary motility disorders suggestive of chronic sinusitis. Investigation of choice is Plain CT scan of nose and paranasal sinus
Treatment:
Medical therapy: Antibiotics with antral irrigation is tried
Surgery:
- Required for ventilating the sinuses
- Endoscopic sinus surgery
- Rarely open procedures like intranasal antrostomy or caldwell luc operation
Fungal Sinusitis
AFRS (Allergic Fungal Rhino Sinusitis)
It is a non-invasive form Caused by Aspergillus. AFRS and Fungal ball does not cause erosion of bone
We use Bent and Kuhn criteria for AFRS which includes:
- Serum IgE level elevated
- KOH stain Positive
- Allergic mucin
- Nasal polyposis
- Double density
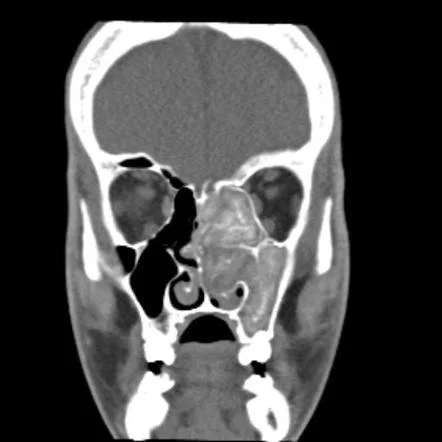
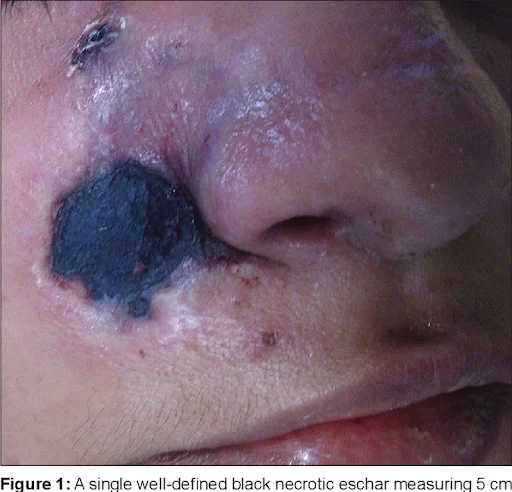
Mucormycosis
This fungus enter into blood vessel and obstruct many blood vessels, no bloody supply causing tissue ischemia which leads to necrosis turning into Black eschar. Causative organism is Angioinvasive fungus. It is Rapidly progressive condition. Black turbinate sign is Seen on MRI (hallmark sign). Radiological IOC: MRI with contrast. Diagnosis is done by histopathology and culture. Treatment is done by Liposomal Amphotericin B + Radical debridement.
Complications of Sinusitis
Types:
- Local: Limited to the sinuses.
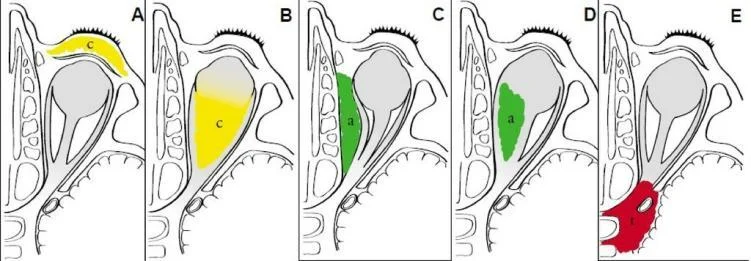
- Maxillary sinus: cystic transformation of mucosa known as Retention cyst. If there is obstruction to the sinus ostium, there will be accumulation of mucus in the sinus with epithelial lined sac around it known as Mucocoele. Mucocoele will gradually expands and cause thinning and destruction of the overlying bone. If mucocoele infected and forms Pyocoele. Infection of overlying bone known as Osteomyelitis
- Orbital
- Preseptal cellulitis
- Cellulitis of skin and subcutaneous tissue: Orbital cellulitis
- Subperiosteal abscess
- Orbital abscess
- Cavernous sinus thrombosis
- Intracranial
- Meningitis
- Extradural abscess
- Subdural abscess
- Brain abscess
- Descending infection
- Adenoiditis
- Tonsillitis
- Pharyngitis
- Laryngitis
| Local | Mucocoele, pyocoele, retention cyst, osteomyelitis |
| Orbital | Chandlers classification |
| Intracranial | Meningitis, abscess |
| Descending infection | Tonsillitis, Pharyngitis, Laryngitis, Tracheobronchitis |
Osteomyelitis of the frontal bone causing subperiosteal abscess known as Pott’s puffy tumor. Orbital cellulitis is particularly common in ethmoid sinusitis.
Mucocoele
It Most commonly involves frontal sinus, Least commonly involves sphenoid sinus. In Frontal sinus mucocoele the Site of infection is superomedial quadrant of orbit. eye is displaced forward, downward, laterally. Cystic, non-tender, egg shell cracking swelling is present. X-ray shows Loss of scalloped margins. Treatment is done by Frontoethmoidectomy to promote drainage of frontal sinus.
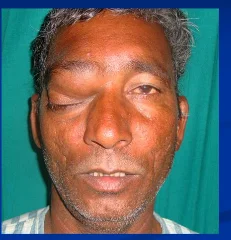
Cavernous Sinus Thrombosis
Infection of ethmoids or sphenoid sinuses is most common cause of cavernous sinus thrombosis,But infection can spread from nose, ear, throat, and orbit. Orbital cellulitis can secondarily lead to cavernous sinus thrombosis.
Also Read: Fungal Sinusitis: Causes, Symptoms, Types, Risk Factors, Diagnosis and Treatment
Cavernous Sinus Thrombosis V/S Orbital Cellulitis
Cavernous sinus thrombosis Orbital cellulitis Source Nose, sinuses, orbit, ear or pharynx Ethmoid sinuses Onset Abrupt with chills and rigors Slow Toxemia Present Late Laterality Bilateral Unilateral Edema of eyelids Bilateral edema of eyelids, chemosis and proptosis Unilateral edema of eyelids, near the inner canthus leading to chemosis and proptosis Cranial nerve involvement Involves individually and sequentially Involved concurrently with complete ophthalmoplegia
Syndromes
Condition Cranial nerves involved Cranial nerves not involved Orbital apex syndrome II, III, IV ±V2 Superior orbital fissure syndrome III, IV, VI±V2 II Cavernous sinus syndrome III, IV, VI II, V2
Download the PrepLadder App and get the best neet pg online coaching with world-class video lectures, QBank, Mock Tests and more!
Download PrepLadder's best app for neet pg preparation for Android
Download PrepLadder's best app for neet pg preparation for ios

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Etiology of Acute Sinusitis
Causes of Acute Sinusitis
Predisposing Factors of Acute Sinusitis
Systemic factors
Bacteriology
Sinusitis Secondary to Dental Infection
Clinical features of Acute Sinusitis
Maxillary Sinusitis
Frontal Sinusitis
Ethmoidal Sinusitis
Sphenoidal Sinusitis
Diagnosis of Acute Sinusitis
Treatment of Acute Sinusitis
Chronic Sinusitis
Fungal Sinusitis
AFRS (Allergic Fungal Rhino Sinusitis)
Mucormycosis
Complications of Sinusitis
Types:
Mucocoele
Cavernous Sinus Thrombosis
Cavernous Sinus Thrombosis V/S Orbital Cellulitis
Syndromes
Top searching words
The most popular search terms used by aspirants
- NEET PG ENT
- NEET PG ENT Preparation
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial