Infections In Pregnancy (Types, Causes, and Treatment)
Mar 2, 2023

Infections in pregnancy are common and a serious problem that can have significant consequences for both the mother and the developing fetus. They can lead to maternal complications such as preterm labor, premature rupture of membranes, and chorioamnionitis. They can also result in adverse fetal outcomes such as congenital anomalies, intrauterine growth restriction, stillbirth, and neonatal sepsis.
For NEET PG aspirants it is important to have a thorough understanding of infections in pregnancy, their diagnosis, management, and prevention. Read this blog further to get a quick overview on this important Obstetrics and Gynecology topic for NEET PG exam.

Vertical Transmission
- Refers to passage of an infectious agent from mother to her fetus through
- The Placenta
- During labor or delivery or
- Breast feeding
- Risk Factors
- Preterm rupture of membranes (PROM)
- Prolonged labor
- Obstetrical manipulations (Like Internal Podalic Version (IPV), Forceps, Vacuum may enhance the risk of Neonatal Infections)
Horizontal Transmission
- Spread of an infectious agent from one individual to another
Secondary Attack Rate
- Probability that infection develops in a susceptible individual following contact with an infectious person.
Viral Infections
Cytomegalovirus
- DNA Herpes virus
- MC perinatal infection in the developing world
- Up to 85% of poor and 50% of higher classes are seropositive by the time of pregnancy.
- Women who develop primary CMV infection during pregnancy [were seronegative before pregnancy], are at greatest risk to have an infected Fetus.
Maternal Infection Features
|
10-15% of infected adults have |
Features of Immuno Compromised |
|
|
Transmission Rates
- 30-36% in 1st Trimester
- 30-40% in 2nd Trimester
- 40-72% in 3rd Trimester
Fetal Infection
(Only 5-10% neonates demonstrate this syndrome)
|
Features |
Complications |
|
|

Periventricular Calcification
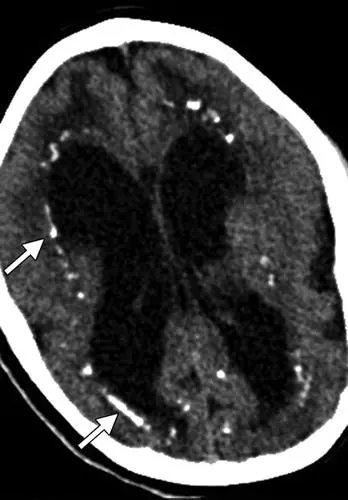
Diagnosis
- Nucleic Acid Amplification Testing (NAAT) of Amniotic Fluid
- Gold standard for Dx of Fetal infection
Management
- Despite the high infection rate with primary infection in the 1st half of pregnancy, most Fetuses develop normally.
- If recent infection is confirmed → Offer Amniotic fluid CMV
- Pregnancy termination may be an option for some
- Oral Valacyclovir 8gm daily is tried on mother
- No Vaccine for CMV is available
Varicella Zoster Infections
- 90% of adults have serological evidence of immunity
- Primary infection → Varicella or Chickenpox
- Transmitted by direct contact with an infected individual
- Incubation period → 10 to 21 days
- 1 to 2 days flu like prodrome followed by Pruritic Vesicular lesion that crust after 3 to 7 days
- Period of communicability → 1 day before the onset of rash until lesions become crusted
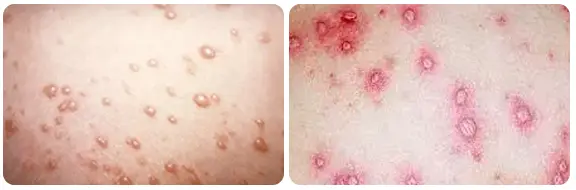
Maternal Mortality
- Predominantly d/t VZV (Pneumonia) in pregnancy
- Risk Factors - Smoking, > 100 cutaneous lesions point towards poor prognosis
- If there is reactivation of primary Varicella years later, it leads to Herpes Zoster or Shingles
- U/L dermatomal Vesicular eruption
- a/w severe pain
- not more frequent or severe in pregnant women
- Congenital Varicella syndrome rarely develops in cases of Maternal Herpes Zoster
Fetal & Neonatal Infection : Congenital Varicella Syndrome
- The highest risk is b/w 13-20 weeks
- Clinical Features
- Chorioretinitis
- Microphthalmia
- Cerebral Cortical atrophy
- Growth restriction
- Hydronephrosis
- Limb hypoplasia
- Cicatricial Skin Lesions
- After 20 weeks of gestation, no clinical evidence of Congenital infection
Around Delivery
- Active infection just before or during delivery (before Maternal antibody formed) is a serious threat.
- Neonatal mortality rate is 30%
- Disseminated Visceral & CNS disease is commonly fatal.
Important Information
- Varicella Zoster Immunoglobulin (VZIG) should be administered to neonates born to mothers who have clinical evidence of Varicella - 5 days before & up to 2 days after delivery.
Diagnosis OF Varicella
Maternal
- Clinical diagnosis
- Confirmed by NAAT of vesicular fluid
- Scraping the Vesicle base & go for Tzanck smear, Tissue culture or Direct Fluorescent antibody testing
Fetal
- Congenital Varicella Dx with NAAT of Amniotic fluid
Management
Maternal Exposure
- Exposed pregnant women who are seronegative should be given VZIG
- Best given with in 96 hrs of exposure
- Can given up to 10 days
Established Maternal Infection
- IV ACYCLOVIR therapy (at 10-15 mg/kg every 8 hrs.) with hospitalization.
Influenza
- Pregnant women are more susceptible to serious complications especially d/t Pulmonary Involvement.
- Orthomyxoviridae → RNA virus → both Influenza A & B cause Epidemics
- Influenza A is not related with congenital malformations
- Viremia is infrequent
- Transplacental passage is rare
- Abortion, Preterm labor, Stillbirth - all reported, but more d/t severity of maternal infection.
- Nasopharyngeal Swabs
- Reverse transcriptase PCR → Most sensitive & specific test
- Rapid Influenza Diagnostic Test (RIDT) → Least sensitive & least indicative
- Treatment
- Neuraminidase Inhibitors
- Oral Oseltamivir for prophylaxis
- Zanamivir inhalation for treatment
- Neuraminidase Inhibitors
Measles & Mumps
- Not Teratogenic
RUBELLA/ GERMAN MEASLES
- RNA Togavirus
Maternal Infection
- Mild febrile illness
- Generalized maculo - papular rash on face & trunk
- 25-50% are asymptomatic
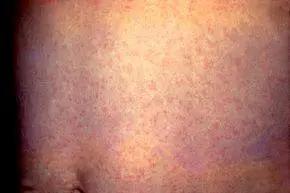
Diagnosis
- ELISA
- IgM antibody detected within 4-5 days of onset of infection
- IgG peaks 1-2 weeks after rash
- High avidity IgG antibodies indicates infection was at least 2 months prior to tests done.
- Most complete Teratogen
- Worse during Organogenesis (1-12 wks of pregnancy)
- Mother to child transmission
- 1st trimester: MTCT → 90%
- 2nd trimester: MTCT → 50%
- End of 2nd trimester: MTCT → 25%
High Avidity IgG Antibodies
- Avidity is the strength of bond of Antibody with Host Cell. i.e. how much strong is the bond
- Loose bond = Low Avidity = Recent infection
- Strong bond = High Avidity = Remote infection
- Done to differentiate Recent positive IgG from Remote positive IgG
- If IgG is positive for long time (Remote positive IgG)↓
- Mother is immune to Rubella & problems in fetus are not likely to happen
- Recent positive IgG (Both IgG & IgM positive)↓
Baby may be affected
Congenital rubella syndrome
Features
- Cardiac septal defects
- Pulmonary stenosis
- Microcephaly
- Cataract
- Hepatosplenomegaly
- Sensorineural deafness
- Intellectual disability
- Neonatal purpura
- Radiolucent bone disease
- Neonates with congenital rubella may shed the virus for many months (threat to others)
- Delayed Morbidities a/w Congenital Rubella Syndrome (CRS)
- Progressive PanEncephalitis
- IDDM
- Thyroid disorders
- Prevention
- Droplet precaution for 7 days after rash
- Can try Passive immunization within 5 days of exposure
- MMR vaccine to all non pregnant women
- Avoid vaccine within 1 month of planning the pregnancy or during pregnancy (as it contains live attenuated virus which can cause defects in fetus)
Vaccines In Pregnancy
|
Contraindicated |
Safe |
|
|
|
Anthrax, Hepatitis A, Japanese Encephalitis, Polio IPV, Yellow Fever are given on special recommendation |
|
ZIKA Virus
- 1st mosquito borne teratogen
- Daytime Aedes mosquito bites
- Family = Flaviviridae
- May have sexual transmission
Maternal Infection
- Rash, Fever, Headache, Arthralgia, Conjunctivitis
- Neurological complications
- Guillain - Barre syndrome, Neuropathy & Myelitis
Fetal Infection (Fetus can be severely affected)
- Birth defects (5-15%)
- Neonatal Deaths (5-7%)
Congenital Zika Syndrome
- Microcephaly
- Lissencephaly
- Ventriculomegaly
- Intracranial calcifications
- Ocular abnormalities
- Congenital contractures
Diagnosis in pregnant women
ZIKA virus in blood & urine
- Do Serological testing & confirm by PCR
- No specific treatment or vaccine of ZIKA so far
Protozoal Infections
Toxoplasmosis
- Feline stage in cats
- Non feline stage in Humans
- Infection is with cat faces or infected meat ingestion
MTCT of Toxoplasmosis
- Rises with increasing gestational age 1
- 1st trimester : 15%
- 2nd trimester: 44%
- 3rd trimester: 70%
Clinically Affected Fetuses have
- Low birth weight
- Hepatosplenomegaly, Jaundice, Anemia
- Neurological diseases with Intracranial calcification, Hydrocephalus, Microcephaly often accompanied by convulsions
- Classical Triad
- Chorioretinitis
- Intracranial calcifications
- Hydrocephalus
Diagnosis
- IgG before pregnancy → No risk
- IgM: appear by 10 days of infection
- Best results are obtained with the Toxoplasma serological profile
- Toxoplasma IgG avidity increases with time
- If high - avidity IgG result is found, infection in the preceding 3-5 months is excluded
Treatment
- Goal of Rx is reduction in rates of serious Neurological sequelae & Neonatal demise
- Spiramycin alone (does not cross placenta)
- Pyrimethamine - Sulfonamide with Folinic Acid (If Fetal Infection is suspected)
Prevention
- Cooking meat to safe temperatures
- Peeling or thoroughly washing fruits & vegetables
- Cleaning all food preparation surfaces
- Wearing gloves when changing cat litter
- Avoiding feeding cats raw or undercooked meat & keeping cats indoors
Malaria In Pregnancy
- Pregnant women have increased susceptibility
- VAR2CSA antigen leads to Antibody formation, which causes accumulation of infected erythrocytes in the placenta, leading to Pregnancy specific Antimalarial immunity
- Higher rates of Maternal Morbidity & Mortality
- Worse in pregnancy
Fetal Infection
- Abortions
- Still birth
- Preterm birth
- Low birth weight
- Congenital malaria (< 5% incidence)
Diagnosis
- Thin & Thick films (Best method)
- Malaria -specific antigens are used for Rapid diagnostic testing but their sensitivity in pregnancy is still an issue
- Anemia is usually same in pregnant women with Malaria d/t significant amount of Hemolysis
Treatment
- Uncomplicated malaria by P. vivax, P. malariae, P. ovale, Chloroquine sensitive Falciparum malaria
- Chloroquine or Hydroxychloroquine
- Complicated P falciparum malaria - Artemisinin based regimens
- Chloroquine resistant P. Vivax - Mefloquine
HIV In Pregnancy
- Mostly by HIV – 1 infection
- Transmitted by
- Sexual intercourse
- Blood transfusion/ Infected needles
- During labor & delivery
- Breast milk
- Primary determinant of transmission → Plasma HIV - 1 viral load
- CD4 site serves as a receptor for virus
- Once infected, CD4 lymphocytes may die
- Illness with AIDS is d/t profound immunodeficiency that gives rise to various opportunities infections and neoplasms
According to CDC, ‘AIDS’ is
- CD4 T cell count < 200 cells/µl
- CD4 T cell count comprising < 14% of all lymphocytes or
- One of several AIDS - defining illness
Screening
- HIV screening using an OPT-OUT approach
- Repeat testing during 3rd trimester is considered for all pregnant women
- Antigen / Antibody combination immuno-assay (Screening Test)
- Detects antibodies against HIV-1 & HIV-2 & HIV-1 P24 Ag.
- If screening test is positive
↓
Do HIV-1 NAAT for confirmation
Vertical Transmission (MTCT Rate → 25-40% overall)
- 1% with < 400 viral copies/ml
- No cases of vertical transmission with maternal viral load <50 copies/ml at delivery
Timing of transmission
- 20% of vertical transmission occurs before 36 weeks
- 50% in the days just before delivery (i.e. 38-39 wks)
- 30% Intra-partum
- Breast feeding MTCT may be as high as 30-40%
Caution
- Didanosine, Stavudine & full dose of Ritonavir are avoided in pregnancy as they are Toxic to mother (not Teratogenic)
- Antiretroviral naive patients are given ART regardless of trimester
- In general, the starting regimen comprises
- 2 Nucleoside Reverse transcriptase inhibitors
Plus - Either a Ritonavir boosted protease inhibitor or an Integrase inhibitor
- 2 Nucleoside Reverse transcriptase inhibitors
- Full dose of Ritonavir is C/I in pregnancy due to its toxicity but Ritonavir boosted protease inhibitors can be given
Recommendations
- Taking ART & pregnant ? Continue current drugs
- All women get ART ASAP? Monitor CD4 count at initial and then 3 monthly visits
- ART Naive
- 2 NRTI
- Abacavir / Lamivudine
- Tenofovir Disoproxil Fumarate / Emtricitabine
- And a Protease Inhibitor
- Atazanavir / Ritonavir
- Or an Integrase Inhibitor
- Raltegravir
- Oral ART during pregnancy + IV Zidovudine during labor can reduce MTCT to < 2 %
Intrapartum Care
- As per NACO & WHO guidelines, there is no benefit of Cesarean section over NVD (Normal Vaginal Delivery)
- C-section is done only in Obstetric indications in an HIV pregnancy
- For HIV RNA > 1000 copies / ml, we can reduce MTCT by giving 2 mg / kg ZDV IV as loading dose then 1 mg/kg hourly till delivery
- For C-section, start IV dose 3 hours prior
Antiretroviral Therapy
- Ideal strategy to suppress viral load & minimize Vertical transmission includes
- Preconceptional ART
- Ante-partum ART
- Intrapartum continuation of Ante-partum Oral ART regimen plus IV Zidovudine
- Newborn ART prophylaxis
PPH in HIV women
- Best managed with Oxytocin and Prostaglandin analogues
- Methylergonovine (Methergine) and other ergot alkaloids adversely interact with Reverse transcriptase inhibitors and Protease inhibitors to cause severe vasoconstriction.
Learn more about infections during pregnancy from experts on the PrepLadder app. Get access to engaging video lectures, comprehensive NEET PG study material and MCQs for practice.

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Vertical Transmission
Horizontal Transmission
Secondary Attack Rate
Viral Infections
Cytomegalovirus
Maternal Infection Features
Transmission Rates
Fetal Infection
Periventricular Calcification
Diagnosis
Management
Varicella Zoster Infections
Maternal Mortality
Fetal & Neonatal Infection : Congenital Varicella Syndrome
Around Delivery
Diagnosis OF Varicella
Maternal
Fetal
Management
Influenza
Measles & Mumps
RUBELLA/ GERMAN MEASLES
Maternal Infection
Diagnosis
High Avidity IgG Antibodies
Congenital rubella syndrome
Features
Vaccines In Pregnancy
ZIKA Virus
Maternal Infection
Fetal Infection (Fetus can be severely affected)
Congenital Zika Syndrome
Diagnosis in pregnant women
Protozoal Infections
Toxoplasmosis
MTCT of Toxoplasmosis
Clinically Affected Fetuses have
Diagnosis
Treatment
Prevention
Malaria In Pregnancy
Fetal Infection
Diagnosis
Treatment
HIV In Pregnancy
Timing of transmission
Caution
Recommendations
Intrapartum Care
Antiretroviral Therapy
PPH in HIV women
Top searching words
The most popular search terms used by aspirants
- NEET PG OBGYN
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial