Regional Anesthesia: Types, Instruments and Side Effects
May 31, 2023

Local or regional anesthesia is given only to the applied region, and in this the patient is fully conscious. For the case of a person with injury in the femur/inguinal hernia/ umbilical hernia, spinal anesthesia is given to the person.
Scale up your NEET PG preparation with this blog on important topics for Anesthesia and experience the best NEET-PG coaching available online.

Types of Local Anesthetic
- Central Neuraxial Blockade comprises a Subarachnoid and Epidural Blockade.
- Local Anaesthesia consists of only Regional anesthesia.
Central Neuraxial Blockade
Layers which are pierced during the administration of the central block are:
Spinal cord → Pia mater → arachnoid mater → dura mater → ligamentum flavum → supra and interspinous ligament → subcutaneous fascia → skin
Between the pia mater and arachnoid mater there is a space known as Subarachnoid space and Between the dura mater and arachnoid mater there is a space known as Subdural space.
From outside to inside,layers are present as skin, subcutaneous fascia, supra and interspinous ligament, ligamentum flavum, dura mater, arachnoid mater, pia mater, and spinal cord. Subarachnoid space contains CSF, whereas Epidural space (outside dura mater) is an air-containing cavity.
Difference between Spinal and Extradural Anaesthesia
Subarachnoid anesthesia is also called spinal anesthesia (giving the drug in the CSF), and epidural anesthesia (air-containing cavity) is also known as extradural anesthesia.
The difference between spinal and extradural anesthesia is given below:
| Subarachnoid / spinal anesthesia | Epidural / extradural anesthesia |
| Drug given is at the level of L2-L5 | Extradural space |
| Fast onset because the drug mixes with CSF | Delayed effect There is no carrier fluid |
| Easy to control the level of the drug with positioning of the patient (drug is hyperbaric) Mixed with dextrose | 1.5-2 ml/ segment To achieve that level of the drug. |
| More haemodynamic imbalance | Less haemodynamic imbalance |
| Easily confirmed with return of CSF | Confirmed with loss of resistance. It require practice |
| Intraoperative use | Since we put an epidural catheter the duration of surgery can be prolonged and can be used for post-op analgesia as well |
Various instruments used during the procedure are shown in the diagram:
|
Needle
|
Needle Touhy’s needle 18 and 16 gaze |
|
S/e- mc complication - hypotension Rx:
Does not increase HR Use in pregnancy
|
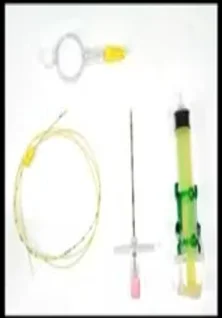

How the instruments are used in giving Central Neuraxial Blockade Anesthesia:
- Tuohy’s needle is put inside the epidural space.
- Lor syringe is used to pump air, and to attain loss of resistance, the syringe is removed.
- The epidural catheter is attached.
- The most commonly used needle is the quincke’s needle.
Side Effect
- Most Common Intraoperative Complication- Hypotension which can be prevented by Preloading (administering 1-2L of fluid before surgery).
- Treatment of hypotension includes IV fluids, IV inotropes, drugs – phenylephrine (best as it does not increase HR and is used in pregnancy), ephedrine, and mephentermine.
- Most Common Postoperative Complication- Urinary retention.
- Other postoperative complications include bradycardia, respiratory distress, high spinal hematoma formation, neurological syndrome, backache, and post-dural puncture headaches.
Contraindications
- Patient refusal is an Absolute Contraindication.
- Localized infections are an Absolute Contraindication.
- A platelet count of less than 50,000 is an Absolute Contraindication.
- Hypovolemia is a relative contraindication.
- Increased intracranial pressure is a relative contraindication.
- Any Kind of heart disease is a relative contraindication.
Special Anaesthetic- Labour Analgesia
In pregnancy, an epidural catheter in epidural space can produce analgesia without giving anesthesia by titrating a dose of local anesthetic. The sensory pathway is blocked, but the motor pathway is normal. Its Composition is Bupivacaine 0.125% + Fentanyl.
Local Anesthetic
Local anesthesia is the condition where there is reversible loss of sensation which is circumscribed to an area by decreasing excitation nerve ending by decreasing conduction. They act by blocking Na+ channels. They consist of aromatic and amino groups which are attached by ester and amide bonds. An active nerve fiber is the best state of a nerve for maximum action of local anesthetic. Systemic absorption:
Intravenous (best) > tracheal > intercostal > paracervical < caudal > lumbar > brachial plexus > sciatic > subcutaneous
Desirable Properties of Local Anaesthetic
- No permanent alteration to nerve fiber.
- Systemic toxicity is low.
- It should have a short onset of action.
- No allergic reaction should be precipitated.
- Not initiating to tissue.
Also Read: Important Topics in Anesthesia for NEET-PG
Different Types of Nerve Fibers
- There are 3 different types of nerves: A (Aα, Aβ, Aγ, Aδ), B, C.
- Fibers most sensitive to local anesthetics are B > C > A
- Desensitization order: autonomic > sensory > motor > temperature > pain > touch > proprioception.
- Reversal is in the opposite direction.
Different Types of Nerve Fibers are given below :
| Different types of Nerve Fibers | |
|---|---|
| A α | Motor |
| A β | Touch, Pressure via Touch |
| A γ | Afferent Muscle Spindles |
| A δ | Fast Pain and Temperature |
| B | Autonomic Preganglionic |
| C | Slow Pain, Post Ganglionic |
Local Anaesthetic Combined with Vasoconstrictor
When a local anesthetic is combined with vasoconstrictor, constriction of vessels and hence less absorption.
| Advantages | Disadvantages |
| Increased duration of drug action | Painful on injection |
| Increased Intensity of action of drug | Tissue edema |
| Decrease systemic toxicity | Necrosis |
| Decrease blood loss |
Groups of Local Anaesthetic and their Classification
It consists of ester and amide groups. Chloroprocaine is the shortest acting. The most widely used are lignocaine, bupivacaine and ropivacaine.
| Ester (i) | Duration | Amides (ii) | Duration |
| Cocaine | Short acting | Lignocaine | Intermediate acting |
| Procaine | Short acting | Mepivacaine | Intermediate acting |
| Chloroprocaine | Shortest acting | Prilocaine | Intermediate acting |
| Benzocaine | Long acting | Bupivacaine | Long acting |
| Tetracaine | Long acting | Ropivacaine | Long acting |
| Dibucaine | Long acting |
- Cocaine- It is the 1ST local anesthetic to be used and has vasoconstrictor properties. It has Natural alkaloids as a property Side effect of cocaine is pyrexia.
- Procaine- It is Topically ineffective and It Produces significant vasodilation causing more systemic absorption, so it has to be combined with adrenaline. It is less potent and has short-duration.
- Lignocaine- It contains an Amide group. It is the safest LOCAL ANAESTHETIC; no allergies and is also an antiarrhythmic drug. It undergoes Hepatic metabolism. It is the DOC of Bier’s block.
- Bupivacaine- It is Added with glucose for spinal anesthesia. It is the most cardiotoxic drug. It is the shorter onset and longer duration. It is used in Labour analgesia. It is the best drug for a differential blockade.
- Ropivacaine- It is less cardiotoxic and It is less potent.
Metabolism of Local Anaesthetic
- Esters: Ester-type local anesthetics are metabolized by plasma pseudocholinesterase and their metabolites. Para-aminobenzoic acid being one of the main. These metabolized products are then excreted through urine. The presence of PABA may cause allergies in some patients. The pathway is the same for all esters containing local anesthetics except cocaine.
- Amide: These are Hydrolyzed by Liver microsomal enzymes, even cocaine.
- Dermal Anaesthetic- Emla Cream
- It contains a mixture of Lignocaine + Prilocaine in (1:1)- 2.5% each. The contact period is 1 hour.
- Last- Local Anaesthetic System Toxicity
Toxicity is highly dangerous, and a scale is present to measure the toxic level called LAST. Symptoms of toxicity include Anxiety, tinnitus, seizures, arrhythmia, and cardiac arrest.
To scale up your NEET PG preparation with the best-in-class video lectures, QBank, Mock Tests and more, download the PrepLadder App!
Download PrepLadder's NEET PG preparation app for Android
Download PrepLadder's NEET PG preparation app for iOS

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Types of Local Anesthetic
Central Neuraxial Blockade
Local Anesthetic
Different Types of Nerve Fibers
Local Anaesthetic Combined with Vasoconstrictor
Groups of Local Anaesthetic and their Classification
Top searching words
The most popular search terms used by aspirants
- NEET PG Anesthesia
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial