Ichthyosis Vulgaris: Types, Causes, Symptoms and Diagnosis
Aug 7, 2023

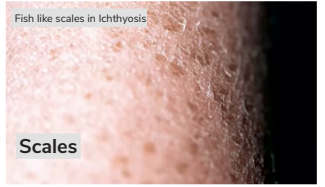
The inherited or acquired skin condition ichthyosis vulgaris may develop when the skin does not exfoliate its dead skin cells. As a result, patches of dry, dead skin cells appear on the skin's surface. The disease is sometimes referred to as "fish scale disease" because the dead skin accumulates in a manner resembling fish scales.
Most occurrences are small and restricted to certain body areas. But in some cases, the back, arms, legs, abdomen, and other large parts of the body are severely affected.

Types Of Ichthyosis
Ichthyosis has more than 20 distinguishing characteristics, some of which co-occur with other syndromes or conditions. Doctors can identify the type of ichthyosis by looking for the:
Alteration to a gene.
Family tree analysis used to determine inheritance patterns.
Details about the symptoms, such as how severe they are and which organs they impact.
Amount of time since the onset of symptoms.
The following are some inherited forms of the illness that are not syndrome-related:
- The most typical type is ichthyosis vulgaris. It typically manifests in the first year of life and causes dry, flaky skin.
- Harlequin ichthyosis. The entire body develops into thick, scaly plates of skin due to harlequin ichthyosis, which is typically visible at birth.
- This kind of illness may restrict joint movement and alter the shape of facial features.
- Epidermolytic ichthyosis manifests at birth. Most newborns have thin skin and blisters all over their bodies at birth. Blisters eventually go away, and skin begins to scale. Over curved parts of the body, this may have a ridged appearance.
- Lamellar ichthyosis manifests at birth. A collodion membrane, which is a tight transparent covering the whole body after birth, is present. The membrane gradually separates, exposing a majority of the body covered in broad, black, plate-like scales.
- Congenital ichthyosiform erythroderma manifests at birth. Additionally, collodion membranes are frequently present in newborns.
- X-linked ichthyosis typically manifests in men between the ages of 3 and 6 months of life. Scaling typically affects the legs, trunk, lower face, and neck, and symptoms might get worse with time.
- Erythrokeratodermia variabilis typically appears a few months after birth and progresses throughout infancy. Usually on the face, buttocks, or limbs, the skin can form rough, thick, or reddish patches. Over time, the skin's afflicted areas may start to spread.
- Progressive symmetric erythrokeratoderma typically manifests as dry, red, scaly skin on the limbs, buttocks, face, ankles, and wrists in childhood.
Also Read: Acne Vulgaris: Classification, Causes, Clinical Presentation, Grading and Treatment
Causes Of Ichthyosis Vulgaris
Like many other skin conditions, ichthyosis vulgaris is hereditarily transmitted. The sickness has an autosomal dominant pattern. This suggests that only one parent needs to carry the faulty gene for the child to inherit it. One of the most common inherited skin diseases is ichthyosis vulgaris.
Adults who don't have the defective gene can nonetheless get ichthyosis vulgaris in a small percentage of cases. Even though it's rare, this commonly coexists with other conditions including thyroid disease, cancer, or kidney failure. It might also be connected to using some prescription medications.
Ichthyosis vulgaris coexist with other skin disorders such as atopic dermatitis or keratosis pilaris. Atopic dermatitis, often known as severe eczema, results in skin rashes that are infamously extremely irritating.
The impacted skin may also be thick and coated in scales. The white or red skin bumps caused by keratosis pilaris often appear on the arms, thighs, or buttocks, despite the fact that they occasionally mimic acne. Another sign of this condition may be areas of rough skin.
Also Read: Melasma: Types, Causes, Risk Factors, Symptoms, Diagnosis, Differential Diagnosis Treatment
Symptoms Of Ichthyosis Vulgaris
Among the symptoms and indicators of ichthyosis vulgaris are:
- Itchy skin and dandruff
- Extremely dry skin is indicated by polygonal, brown, grey, or white scales on the surface of the body.
- Enlarged skin
The symptoms of ichthyosis vulgaris frequently worsen in the wintertime when the air is colder and drier. The usual places for dry skin patches to appear are the elbows and lower legs. It usually shows up as large, black patches on the shins.
Ichthyosis vulgaris can appear at birth or progress over the first several years of a child's life. It typically disappears during early childhood. Some people may never experience symptoms again. However, some people might have a recurrence as adults.
Also Read: Urticaria: Classification, Causes, Symptoms, Complications, Diagnosis, Treatment and Prevention
Diagnosis Of Ichthyosis Vulgaris
Ichthyosis vulgaris is commonly misdiagnosed as normal dry skin because of how frequently it looks like that. If using moisturizer twice daily is ineffective, a dermatologist can identify ichthyosis vulgaris by inspecting the skin and separating it from other skin conditions.
Prior to visiting the doctor:
- See if any of your family relatives have comparable skin issues.
- Note when the symptoms first started to show up.
- Make a note of your current drugs, vitamins, and supplements, as well as any additional skin or medical concerns you may have.
- The physician might take a biopsy (remove a small section of skin for microscopic examination). The doctor can also recommend a genetic test because the condition is inherited in offspring.
Also Read: Leprosy Symptoms, Treatment, Types, Causes, Diagnosis

Treatment Of Ichthyosis Vulgaris
Ichthyosis vulgaris has no known treatment, however, individuals sometimes find comfort in the scaly, dry skin. Your physician might advise you to take the following actions:
- More than once a day, take a bath. Scales become softer when the skin is moisturized.
- Apply petroleum jelly or other thick, bland emollients to open sores or large cracks before taking a bath. Such creams can heal deep skin fissures and reduce any burning or stinging that the water may produce. Sea salt can help soothe burning, stinging, and itching.
- Apply generous amounts of moisturizer right away after taking a bath. A moisturizer can help your skin retain moisture after a bath. Additionally, some powerful moisturizers that contain the substances lactic acid, salicylic acid, and urea can aid in normal skin shedding.
- Take the prescribed oral and/or topical treatments, such as antibiotics for skin infections, as directed by your doctor.
- If skin infections are common, add a small amount of bleach to the bathwater. The amount of bacteria on the skin is reduced with bleach. (Only follow a doctor's instructions if this step is advised.)
- After the bathwater has softened the scales, gently rub them with an abrasive sponge while still in the tub. Dead skin will be eliminated in this way.
- Reduce the dosage of the medicine or treat the underlying illness that led to acquired ichthyosis vulgaris.
Complications Of Ichthyosis Vulgaris
The following are ichthyosis vulgaris complications:
- Skin infections
- Children who have the condition may be more likely to develop eczema, asthma, hay fever, and hives.
- Dehydration, scorching, excessive heat, calorie loss that happens quickly, and skin allergies can all be brought on by ichthyosis vulgaris.
- The appearance of the skin may also cause a patient to experience psychological harm.
Also Read: Angioedema : Symptoms, Causes, Types, Diagnosis and Treatment
Download the PrepLadder App and get the best neet pg online coaching with world-class video lectures, QBank, Mock Tests and more!
Download PrepLadder's best app for neet pg preparation for Android
Download PrepLadder's best app for neet pg preparation for ios

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Types Of Ichthyosis
Causes Of Ichthyosis Vulgaris
Symptoms Of Ichthyosis Vulgaris
Diagnosis Of Ichthyosis Vulgaris
Treatment Of Ichthyosis Vulgaris
Complications Of Ichthyosis Vulgaris
Top searching words
The most popular search terms used by aspirants
- Medical PG Dermatology
- NEET PG Dermatology
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial