Pulmonary Embolism: Causes, Symptoms, Diagnosis & Treatment
Jul 19, 2023

A pulmonary embolism is a blood clot that prevents blood flow to a lung artery. Most frequently, a blood clot begins in a deep leg vein and moves to the lung. Rarely does the clot develop in a vein in a different area of the body. Deep vein thrombosis (DVT) is the medical term for when a blood clot develops in one or more of the body's deep veins.
Pneumoembolism poses a serious risk to life because one or more clots prevent blood from reaching the lungs. But the chance of dying is significantly decreased with quick medical attention. You can lessen your risk of pulmonary embolism by taking steps to avoid blood clots in your legs.

Causes Of Pulmonary Embolism
Blood clotting occurs naturally to stop bleeding. Blood clots are formed by the body, which then dissolves them. In some cases, the body may not be able to dissolve a clot. A significant health issue could come from this.
It is possible for blood to clot in a vein as a result of decreased blood flow, a defect in clot formation, or damage to the blood vessel wall.
In arteries and veins, blood clots can develop. Leg veins can either be deep veins, which are encircled by muscle and bone, or superficial veins, which are close to the skin's surface.
Deep leg veins are where venous clots most frequently form. Deep vein thrombosis (DVT) is the medical term for this condition. Once a blood clot has developed in the deep veins of the leg, there is a chance that some of it could separate and move through the circulation to another part of the body, frequently the lung. A pulmonary embolism is most frequently caused by DVT.
Deep vein thrombosis: “Virchow Triad”. Prolonged Immobilization for more than 72 hours can cause thrombosis in mainly soleal veins and popliteal veins so a piece of the clot has broken and passes through the right side of the heart resulting in a ventilation-perfusion mismatch.
Prothrombotic state:
- Autosomal dominant conditions like Factors V Leiden mutation and Prothrombin Gene mutation
- Antiphospholipid syndrome- Anti β2 glycoprotein antibody is the troublemaker in this. It Stimulates the intrinsic pathway.
- Oral contraceptives
- Hormone replacement therapy in post-menopausal female
- Cancer surgery: Cancer surgeries can be a disaster. Because cancer is a hypercoagulable state. After the removal of cancer, the clot can be formed.

- Ortho implant surgeries (Massive PE can develop on 3rd postoperative day)
A fat embolus (typically related to the shattering of a big bone), an embolus of amniotic fluid, air bubbles, and an upper body deep vein thrombosis are some less common causes of pulmonary embolism. Additionally, clots may develop on the end of an intravenous (IV) catheter that is inserted continuously, separate, and go to the lungs.
Symptoms Of Pulmonary Embolism
The signs of a pulmonary embolism can be very different depending on how much of your lung is damaged, the size of the clots, and whether or not you have a heart or lung condition.
These are typical symptoms:
- Difficulties Breathing. It usually comes on suddenly with this illness. Breathing is challenging even when you're at rest, and exercising only makes it worse.
- A Chest Pain. A heart attack might manifest as symptoms. You frequently experience extreme pain when taking a deep breath. There's a chance that the pain will prevent you from taking a deep breath. You may experience it when you cough, stoop down, or lean back.
- Fainting. If your blood pressure or heart rate decreases suddenly, you could faint.
Also Read: Sjogren's Syndrome: Causes, Symptoms, Risk Factors, Diagnosis, Treatment and Complications
Other Signs of Pulmonary Embolism Include:
- A cough that could produce blood or blood-stained mucous
- Rapid or irregular heartbeat
- Dizziness or lightheadedness
- An excessive amount of sweating
- Fever
- Typically in the back of the lower leg, leg discomfort, edema, or both
- Skin that is clammy or discolored is referred to as cyanosis.
Also Read: Heartburn: Causes, Symptoms, Diagnosis, Treatment and Complications
Risk Factors For Pulmonary Embolism
Pulmonary embolism risk factors include:
- Circumstances genetically predisposed to the development of blood clots
- A history of blood clotting issues in the family
- Orthopaedic surgery, injury (particularly to the legs), or both
- Situations that restrict mobility, such as prolonged bed rest, long flights or rides, or paralysis
- Previous clot history
- Older age
- Cancer treatment and cancer
- Several illnesses, including inflammatory bowel disease, high blood pressure, chronic obstructive pulmonary disease (COPD), and heart failure
- Several drugs, including birth control pills and oestrogen replacement treatment
- When pregnant and after, including after a caesarean section
- Obesity
- Smoking cigarettes
Examination
On examining the patient with pulmonary embolism we can find the following findings:
- Heart rate is 120/min, BP 90/60 mmHg and JVP elevated.
- Kussmaul sign present S1 Loud
- S2 wide fixed split because P2 closure takes more than 30 msec.
- Heard with diaphragm S3 ⊕
- Lungs: Bilateral clear lung fields
Well’s Criteria
The Wells criteria for pulmonary embolism is a risk stratification score and clinical decision rule used to calculate the likelihood of acute pulmonary embolism (PE) in individuals whose medical histories and physical examinations suggest that acute PE may be present. It includes the following:
B – Blood in sputum
D – Deep vein thrombosis sign and symptoms present is Homan Sign (Pain on the calf while dorsiflexion of the ankle)
C – Cancers
H – A heart rate of more than 100 /min on the 3rd or 4th day is suggestive of atelectasis or PTE.
I – Immobilization of more than 3 days or surgery less than 4 weeks
P– Prior pulmonary embolism Or Prior DVT (If Score > 4 = High probability)

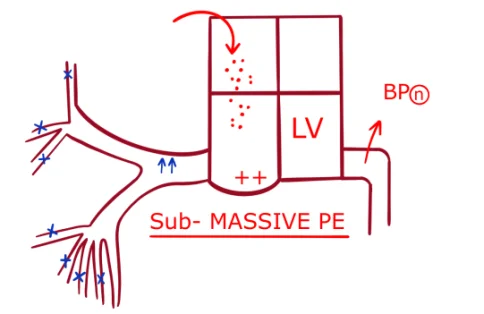
Sub-Massive Pulmonary Embolism
Multiple small pulmonary emboli enter into the Right heart leading to blockage of small arteries of the Pulmonary artery that result in mild distension of the right ventricle without affecting the left ventricle. Seen in around 60 % of cases. In this condition, the Blood pressure tends to remain normal in the patient.
Also Read: Dupuytren Contracture: Causes, Symptoms, Risk Factors, Diagnosis and Treatment
Diagnosis Of Pulmonary Embolism
Diagnosis of pulmonary embolism can be made with the help of following methods:
- E.C.G = S1 Q3 T3
- Deep S wave in lead I
- Deep Q wave in lead III shows RV Strain pattern
- Inverted T wave in lead III
- Chest X-ray
- Palla sign
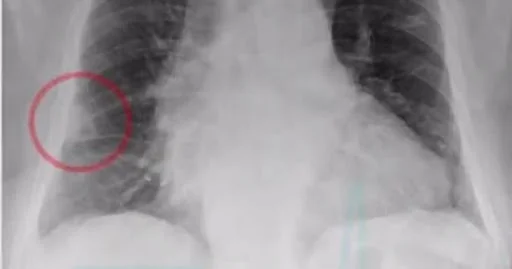
- Hampton hump
- Wester mark sign
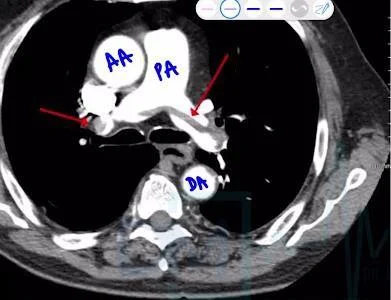
There is a block by dislodged emboli on the pulmonary artery which presents dilated to the proximal emboli called Palla sign - commonly seen in the Right descending pulmonary artery and wedge-shaped infarction to the distal emboli called Hampton hump.
Wester Mark Sign – Due to focal oligemia seen in only one lung where emboli lodged into the Right descending pulmonary artery.

- Trop I or HFABP or B.N.P: Elevated due to Right ventricular micro infarction
- USG or Doppler of legs: Noncompressibility of big veins (normally these veins are compressed by placing the USG probe)
- Screening test: D – Dimer assay elevated.
- Investigation of choice is CT angiography
Also Read: Leukemia: Causes, Symptoms, Classification, Types, Risk Factors, Diagnosis and Treatment
Treatment Of Pulmonary Embolism
Pulmonary embolism (PE) treatment options include:
- Anticoagulants. These drugs, which are also known as blood thinners, lessen the blood's capacity to clot. This aids in preventing blood clots from growing larger and from developing new ones. Heparin and warfarin are two examples.
- Fibrinolytic treatment. These drugs, also known as clot busters, are administered intravenously (IV or into a vein) in order to dissolve the clot. Only life-threatening conditions should be treated with these medications.
- Ventricle filter. To prevent clots from reaching the lungs, a small metal device may be implanted in the vena cava, a large blood artery that returns blood from the body to the heart.
- These filters are typically utilised when anticoagulation treatment is not an option (due to a medical condition), when anticoagulation treatment results in the formation of more clots, or when anticoagulation medication causes bleeding issues.
- Embolectomy of the lungs. This is a procedure that is used infrequently to eliminate a PE. It is typically only used in extreme situations where the PE is very large, you can't receive anticoagulation or thrombolytic therapy because of another medical condition or you haven't responded well to it, or your condition is unstable.
- Thrombolysis using a needle. In order to reach the embolism site, a long, thin, hollow tube (catheter) can be inserted through the blood vessel under X-ray guidance. Once the catheter is in position, the embolism is broken up, pulled out, or eliminated utilising it.
Also Read: Infectious Mononucleosis: Causes, Symptoms, Diagnosis, Treatment, Prevention and Complications
Download the PrepLadder App and get the best neet pg online coaching with world-class video lectures, QBank, Mock Tests and more!
Download PrepLadder's NEET PG preparation app for Android
Download PrepLadder's NEET PG preparation app for iOS

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Causes Of Pulmonary Embolism
Symptoms Of Pulmonary Embolism
Other Signs of Pulmonary Embolism Include:
Risk Factors For Pulmonary Embolism
Examination
Well’s Criteria
Sub-Massive Pulmonary Embolism
Diagnosis Of Pulmonary Embolism
Treatment Of Pulmonary Embolism
Top searching words
The most popular search terms used by aspirants
- NEET PG Medicine
- NEET PG Medicine Preparation
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial