Cell Injury and Cell Death
Feb 19, 2025

In reaction to injury, the cell goes through a number of modifications that might or might not result in cell death. The process of cellular adaptation, which cells engage in to endure the adverse changes in their environment, is triggered by harmful stimuli. Cell damage results from overworked adaptive systems. Reversible damage is caused by mild stressors. Injury becomes irreversible if the stimulus is strong or prolonged. The cell membranes, mitochondria, protein synthesis machinery, and DNA are the main targets of cell damage.
DNA-a deoxyribonucleotide polymer that serves as the foundation for all cells' genetic makeup. Although DNA in eukaryotic and prokaryotic organisms is typically double-stranded, several crucial biological processes briefly involve single-stranded regions.
Cell death is a result of numerous cellular abnormalities brought on by the damage. Necrosis and apoptosis are the two primary forms of cell death.
Necrosis is a pathological cell death associated with inflammation whereas apoptosis is a Programmed cell death and it can occur due to both physiological or pathological causes.
Read this blog further to get a quick overview of this important topic for pathology and ace your NEET PG exam preparation.

What is Cell Injury?
Cell injury occurs when the maximum adaptive response to physiologic or pathologic stimuli is exceeded or cells are unable to adjust. It occurs in relation to harmful stressors, nutritional loss, or mutations.
Types of cell injury
There are 2 types of cell injuries
- Reversible cell injury: In this the morphologic and functional damage changes of the cell are reversible if the cause of injury is removed.
- Irreversible injury and cell death: In this the morphologic and functional damage changes of the cell are not reversible and it is due to continuing damage of the cell which leads to death of the cell.
Causes of cell injury are
- Hypoxia or a lack of oxygen: it is the most common cause of cell injury.
- Physical and chemical threats (radiation, heat, cold, acids, alkalis, and poisonous gases).
- Disorders & nutritional deficits.
- Biological and microbial agent.
- When a cell is injured, it may develop a new morphology that can be reversed. These alterations can take the shape of hydropic, fatty, or hyaline modifications. If the changes are permanent, they might manifest as autolysis, necrosis, or apoptosis, among other things. If a cell dies following injury, gangrene or pathological calcification may result.
- After being damaged, certain cells develop the following illnesses.
- Atrophy, which is a reduction in cell size brought on by physiological or pathological conditions
- Hypertrophy is the enlargement of cells as a result of physiological or pathological situations.
- Metaplasia, which is the transient conversion of one type of cell into another
- Dysplasia: also known as atypical hyperplasia. In this there is permanent conversion of one type of cell to another.
Hypoxia is the most important cause of cell injury whereas the most common cause of hypoxia is ischemia.
Cells which are most resistant to hypoxia are brain cells. Continuous hypoxia of 3-5 minutes leads to death of brain cells.
Cells which are most resistant to hypoxia are fibroblasts.
What is Reversible cell injury?
Due to hypoxia there is mitochondrial dysfunction as we know that mitochondria is the powerhouse of the cell. This leads to decrease in atp production.
This decrease in atp production leads to:
- Failure of sodium potassium pump
- Anaerobic glycolysis
- Decrease in protein synthesis
Failure of sodium potassium pump
In a normal cell there is exchange of three sodium to two potassium i.e. 3 na move out of the cell whereas 2 potassium enters inside the cell. This exchange of ions occurs with the help of ATP. In case when there is decrease in ATP synthesis then this pump stops working and now three sodiums will be moving inside the cell whereas two potassium will be going out. As a result there will be more ions inside the cell due to which the water starts moving inside the cell leads to cellular swelling. This is known as hydropic change and also the 1st morphological change which can be seen in cell injury.
Due to this cellular swelling the organelles inside the cell also start to swell and then the endoplasmic reticulum also swells up and the microvilli present on the surface of endoplasmic reticulum flattens this is known as flattening of endoplasmic reticulum.
Cytoplasmic blebs can also be seen due to excessive amount of water inside the cell.
Myelin figures
These are derived from membranes of the cell. These are concentric lamellations which are made up of phospholipids and calcium.
Myelin figures are seen in both reversible and irreversible cell injury.
- Anaerobic Glycolysis:
Due to decrease in ATP production there is excessive accumulation of lactic acid which leads to decrease in ph i.e it becomes more acidic and it leads to nuclear chromatin clumping.
- Rough Endoplasmic Reticulum:
Due to decrease in atp the ribosomes which are attached on the surface of endoplasmic reticulum detached which leads to further decrease in protein synthesis and there will be excessive accumulation of fat so this is known as the fatty change.
On microscope the hydropic change in kidney appears as cloudy swelling kidney as due to entry of excessive amount of water the cells of the kidney starts to appear as white.
What is Irreversible cell injury?
There are 2 defining moments in irreversible cell injury:
1. Severe membrane damage
2. Severe mitochondrial damage
Severe membrane damage
The membrane is the barrier which prevents certain substances to directly enter inside the cell. When the membrane of the cell is damaged then there is influx of calcium inside the cell and this calcium activates the enzyme as calcium is the cofactor for enzyme activation. It activates phospholipase, nuclease and protease which leads to cell death. Calcium enters inside the cell and attaches to mitochondria, this is known as amorphous flocculent densities.
Nuclear change of the cell in irreversible cell injury:
Normal cell
↓
Pyknosis
↓
Karyorrhexis
↓
Karyolysis
Pyknosis: Shrinkage of chromatin material is known as pyknosis
Karyorrhexis: The irreparably broken down nucleus of a dying cell, with its chromatin dispersed erratically throughout the cytoplasm.
Karyolysis: Complete destruction of chromatin material is known as karyolysis.
Also Read:
Henoch- Schonlein Purpura : Causes, Symptoms, Pathophysiology, Diagnosis, Treatment and Prognosis
Trisomy 18: Causes, Symptoms, Types, Diagnosis, Treatment and Prevention : Pathology
Cell Death
Necrosis
Pathological cell death associated with inflammation. It is a passive process i.e. it does not require ATP. Morphological changes in a tissue after cell death occurs
Types of necrosis
Coagulative necrosis
- It is the most common type of necrosis seen microscopically
- MC cause of coagulative necrosis ischemia
- Denaturation of proteins, inactivation of hydrolytic enzymes and intact structural outline.
- Neutrophilic infiltration is classically noted in Coagulative necrosis (for clearing dead cells
- Coagulative necrosis is associated with "Tombstone Appearance" → can be seen in all organs except CNS.
- It is also Seen in Zenker's degeneration → coagulative necrosis in skeletal muscle, associated with typhoid infection.
Infarct
Localized area formed due to ischemia, usually triangular in shape. Apex of infarct points in the direction of site of obstruction.
Subtypes of Infarct
- White Infarct: It is Seen in organs with end-arterial blood supply, particularly in solid organs Eg: Heart, Kidneys.
- Red Infarct: It is Seen in Organs with loose Connective tissues
Liquefactive/Colliquative Necrosis
Hydrolytic enzyme activation causes damage to tissues (liquefied) in this Structural outline not preserved microscopically · Examples
CNS Ischemia → damage to glial cells leading to hydrolytic enzyme activation
Infections → associated with pus formation in Staphylococcus aureus infection
Caseous necrosis
- 'Cheese - like' necrotic material. It is actually a combination of Coagulative and liquefactive necrosis, with coagulative necrosis being the predominant contributor.
- Seen in organisms with high lipid content like TB. It is also seen in other conditions like fungal infections (Histoplasmosis, coccidioidomycosis) and syphilis. · Granulomatous reaction present.
- Microscopic appearance: Langhans Giant cell/monocytic/lymphocytic infiltrates are seen which are Associated with tubercular focus
Fat necrosis
It is Associated with organs with high fats or with high concentration of lipases.
Seen with injury to breast tissue, omentum tissue injury and pancreatitis Acute Pancreatitis
GallStones / Alcohol
↓
Lipase activation
↓
Lipids
↓
Fatty Acids + Ca
↓
Saponification ('Chalk-like' yellow white deposits)
Sr. Ca level (↓↓) is an important prognostic factor to assess the severity of pancreatitis.
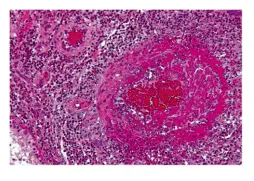
Fibrinoid Necrosis
Endothelial Cell Injury
↓
Immune Complex formation
↓
Entry or leakage of plasma protein to the vessel wall
↓
Inside the vessel wall (seen as pinkish appearance in the vessel), there is deposition of plasma protein
↓
Fibrinoid Necrosis
Also Read:
Gangrene
- Blackish discoloration of organs giving a foul smell.
There are 2 types of gangrene
- Dry gangrene: It shows coagulative necrosis line of demarcation is present .It occurs due to blood vessel occlusion.
- Wet gangrene: It shows liquefactive necrosis. Occurs due to blood vessel occlusion and infection so no line of demarcation present.

- Can be seen in
- Malignant Hypertension
- Aschoff Body in cardiac tissue
- Immune Complex Disorder/Type 3 Hypersensitivity Reaction (PAN/HSP)
Zenker's Degeneration:
- It is a type of Coagulative Necrosis.
- It occurs in typhoid or Enteric fever.
- Complication seen in: Recuts abdominis and diaphragm
Apoptosis
Apoptosis is a type of caspase-dependent programmed cell death. · It is controlled by genes, and it affects a single cell or a small group of cells.
|
Pro-apoptotic genes |
Anti-apoptotic genes |
Sensors |
|
|
|
Physiological Apoptosis is seen in
- Embryogenesis
- Removal of tail cells present in developing fetus
- Separation of fingers due to death of cells present between fingers. If apoptosis fails to occur, fingers will not separate resulting in a condition known as Syndactyly.
- Females of Reproductive Age group- During menstrual cycle, hormone (Estrogen) promotes formation of new layers of endometrium and shedding, as per its levels in various parts of the cycle.
- Self-Reactive B & T Cells
Pathological apoptosis is seen in
- DNA Damage → in response to a person's exposure to radiation or drugs.
- Viral infections of hepatitis → “Councilman Body
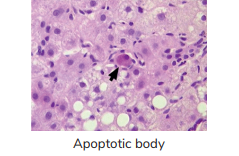
Pathways in Apoptosis
Intrinsic / mitochondrial pathway
Growth factors
↓
BCL-2 inactivation
↓
BCL-2 replaced by BAK / BAX
↓
Mitochondrial permeability
↓
↑ Cytochrome-C in cytoplasm
↓
Activation of APAF-1 (Apoptosome)
↓
↑ Activation of Caspase 9
↓
Stimulate Caspase 3/ 6/ 7
↓
↑ Activation of Proteases & Endonucleases
↓
Cell Death
Extrinsic pathway:
FAS –L / TNF α Release (in severe damage)
↓
FAS –L / TNF α + FAS –L / TNF-R
↓
Trimerization ↓ Activation of FADD
↓
Pro CASPASE 8/ 10 → Caspase 8/ 10
↓
↑ Activation of Caspase 3 /6 /7
↓
↑ Activation of Proteases & Endonucleases
↓
Cell Death
Abbreviations
- APAF-1 → Apoptosis Activating Factor 1, also called as apoptosome
- FADD → Fas Associate Death Domain ·
- IAP → Inhibitor of Apoptotic- protein, inhibits intrinsic pathway.
Caspases
Cysteine containing special proteases acting on targets at the aspartic acid residues.
| Caspase Type | Intrinsic pathway | Extrinsic pathway |
| Initiator | Caspase 9 | Caspase 8 (Worms), Caspase 10 (Humans) |
| Executioner | Caspase 3/6/7 | Caspase 3/6/7 |
Efferocytosis
- The apoptotic bodies express eat-me signals through C1q, Thrombospondin and PS (Phosphatidyl Serine).
- In a normal cell, Phosphatidyl Serine is found in the inner leaflet. However, in apoptotic cells, it comes out.
- There is Phosphatidyl Serine Flipping.
- The flipping of PS is a signal for the Macrophage. A defect in this process results in Scott Syndrome.
- The Macrophage engulfs the apoptotic bodies, which is called Efferocytosis.
Defects in Efferosome
- SLE
- COPD
- Bronchiectasis
- Cystic fibrosis
- Survival of Cancer cells:
- Cancer cells express CD47 ("Do not Eat me" Signal) to Macrophages.
Update Robbins 10e-
- Pro apoptotic molecules [BAK, BAX, BCL XS]: BH 1 - 3
- Anti-apoptotic molecules [BCL2, MCLI, BCL XL]: BH 1 - 4
- Stress sensors [BIM, BID, BAD, NOXA, PUMA]: BH 3 only
- SMAC / DIABLO: Proapoptotic
- Glucocorticoids: Proapoptotic
- Sex Steroids: Antiapoptotic
Identification of Apoptosis
- Marker: Annexin V (marker for testing PS flipping)
- Molecular Marker: CD95/ Fas
- Microscopic Examination: Nuclear Chromatic Condensation. (The cytoplasm will be pink and Nucleus will be blue, along with cellular shrinkage)
- Stain: Tunel Stain (TdT dUTP Nick End Labelling)
- Positive: Apoptosis
- Negative: Necrosis
- Gel Electrophoresis: Step Ladder Apoptosis
Smearing: Referred to the DNA gel Electrophoresis, where the ink smudges till the end continuously. Smearing is seen only in Necrosis whereas Step Ladder is seen both in Apoptosis and Necrosis. As Neuronal cells don't have caspases, the hallmark of neuronal apoptosis is AIF(apoptosis- inducing factor).
FAQs
Q. What is the most common type of Necrosis?
Ans. Coagulative Necrosis
Q. Which are the most common organs affected by Coagulative Necrosis?
Ans. Heart
Q. Which necrosis happens inside the pancreas?
Ans. Liquefactive Necrosis
Q. Which necrosis happens around the pancreas?
Ans. Fat Necrosis
Q. Zenker's Degeneration can be seen in which skeletal muscles?
Ans. Rectus Abdominis and Diaphragmatic Muscle
Q. What is the first change in the cell injury?
Ans. Mitochondrial Dysfunction
Q. Which is the first morphological change in the cell injury?
Ans. The cellular swelling or Hydropic Change.
Q. What is the composition of Myelin Figures?
Ans. Primarily made up of phospholipids and a minor presence of calcium.
Q. What is the composition of Amorphous Flocculent Densities?
Ans. Calcium
Q. The injury with which the Amorphous Flocculent Densities are associated?
Ans. Irreversible Cell Injury
Q. The three stages of nuclear change in the cell injury?
Ans. Pyknosis, Karyorrhexis and Karyolysis
Salient Features of Apoptosis
Cell shrinkage: Cell size decreases due to damage to structural proteins.
Chromatin Condensation
- Caused due to endonuclease activation
- Hallmark feature associated with apoptosis ·
No cell membrane damage as there is no activation of phospholipase enzyme.
No Inflammation Tests to Detect Apoptosis.
Tunel Technique
- It is Used for diagnosis of apoptosis
- dUTP dye is used and fragments of DNA are visualized by light microscope ·
Gel Electrophoresis
In gel electrophoresis we can detect the type of cell injury.
- Apoptotic nucleic acid are found to be in Step-Ladder Pattern.
- Necrosis nucleic acid are found in smearing pattern.
Staining
It is Done by using ANNEXIN 'V' which attaches to flipped molecules or by using DAPI Stain.
- Molecules which can flip over, and hence are expressed more at the time of apoptosis, include:
- Phosphatidylserine
- C1q
- Thrombospondin Clinical Significance of Apoptosis
- Excessive apoptosis is seen in
- Neuro-degenerative disorders
- Viral infections
- Reduced apoptosis is seen in
Pyroptosis
- It is a special type of apoptosis, with noted cellular swelling and inflammation.
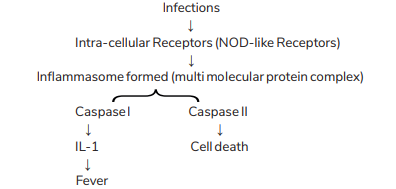
- Other Caspases which have an action similar to Caspase 1 would be Caspase 11, 4 and 5.
- Efferocytosis is the name of the process through which molecules like C1q and Thrombospondin attract phagocytes during apoptosis.
Necroptosis/ Programmed Necrosis
It is a Caspase-Independent programmed cell death.
TNF + TNF-
↓
RIP 1 / 3 [Receptor Interacting Protein Kinase]
↓
Phosphorylation of MLKL Protein
↓
↓PM damage & Inflammation ⊕
Conditions where necroptosis is seen
o Physiological→ Mammalian Growth Plate
Pathological → Pancreatitis, Reperfusion injury, Parkinsonism, Steatohepatitis
Also Read: Amyloidosis: Types, Causes, Symptoms, Diagnosis, Risk Factors, Treatment
This is everything that you need to know about hyperthyroidism for your pathology preparation . For more interesting and informative blog posts like this download the PrepLadder App and keep reading our blog!

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
What is Cell Injury?
Types of cell injury
Causes of cell injury are
Stage of cell injury
What is Reversible cell injury?
Failure of sodium potassium pump
Myelin figures
What is Irreversible cell injury?
Severe membrane damage
Cell Death
Necrosis
Types of necrosis
Coagulative necrosis
Infarct
Subtypes of Infarct
Liquefactive/Colliquative Necrosis
Caseous necrosis
Fat necrosis
Fibrinoid Necrosis
Gangrene
Zenker's Degeneration:
Apoptosis
Physiological Apoptosis is seen in
Pathological apoptosis is seen in
Pathways in Apoptosis
Abbreviations
Caspases
Efferocytosis
Defects in Efferosome
Update Robbins 10e-
Identification of Apoptosis
FAQs
Salient Features of Apoptosis
Tunel Technique
Gel Electrophoresis
Staining
Pyroptosis
Necroptosis/ Programmed Necrosis
Conditions where necroptosis is seen
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial
