Inflammation Types - NEET PG Pathology
Feb 9, 2023

Inflammation is an important topic for NEET PG exam preparation because it is a fundamental process in the human body that plays a critical role in maintaining homeostasis and protecting against infection, injury and disease. Inflammation is involved in a wide range of medical conditions, such as autoimmune diseases, cardiovascular disease, cancer, and many others. Understanding the mechanisms and consequences of inflammation is crucial.
Read this blog further to strengthen your preparation of Pathology for NEET PG Preparation.

Overview
Response of the vascularized connective tissue to noxious stimulus.
Types of inflammation
Following are the different types of inflammation -
- Serous
- Mucinous
- Purulent
- Fibrinous
- Catarrhal: It is the commonest pattern of inflammation that is seen clinically is catarrhal: Associated with leakage of mucin & fluid.
Inflammation can be acute or chronic.
- Acute: Short duration
- Chronic: Long duration
Acute inflammation
Acute inflammation has 2 components -
1. Vascular changes: seen in vessels.
2. Cellular changes: seen in WBCs.
1. Vascular changes: Seen in Small vessels
- Vasoconstriction (earliest vascular response to any injury is vasoconstriction).
- Vasodilation: Commonest chemical mediator contributing to vasodilation is histamine.
- Increased vascular permeability: This is the most characteristic vascular change associated with inflammation. Most common vessels affected is post-capillary venules.
- Mechanism of increased vascular permeability
- Endothelial cell contraction (Commonest Mechanism) → (Immediate transient response) e.g., vasodilation or increased permeability associated with thorn prick.
- Direct Endothelial cell injury: Immediate sustained response. Seen in severe burns, septicemia.
- Endothelial cell retraction: It is a delayed transient response. Seen in Cytokine mediated injury, hypoxia, Bacterial infections
- Endothelial cell damage: It is a delayed prolonged response. Seen in late developing sunburn & radiation
- Stasis: Reduction in velocity blood flow.
2. Cellular changes
- Intravascular
- Extravascular
Intravascular
- Margination: It is movement of WBC from centre toward periphery.
- Rolling: loose adhesion of WBC with endothelial cell. Rolling is dependent on special molecules which are called selectins, selectins interact with sialyl-Lewis X present on WBCs.
- Example of selectins: ‘p’ selectin source-Weibel Palade body of endothelial cells
- Weibel Palade body containing VWF, ‘P’ selectin.
- Adhesion: Firm adhesion of WBC with endothelial cells. Molecules needed for firm adhesion are integrins. Integrins are present on WBCs, and they interact with the receptors on endothelial cells named as intercellular adhesion molecule (ICAM) and vascular cell adhesion molecule (VCAM). Defects in integrins lead to LAD 1 defect.
Also Read: Thalassemia - Symptoms and Causes - NEET PG Pathology
Leukocyte Adhesion deficiency disorders (LAD)
- LAD 1
- Seen in defects of integrins (CD11 or LFA) or Adhesion molecules.
- H/O, Delayed separation of Umbilical cord at time of birth and recurrent infection. (recurrent infections occur because WBCs are unable to reach the site of infection.
- There is presence of neutrophilia and minimal Pus formation.
- LAD 2
- Occurs due to defects in selections.
- Features include short stature, presence of Bombay blood group
- Recurrent infections are common finding in both LAD 1 and LAD 2
- H/O rarest blood group – Bombay blood group, short stature.
- Diapedesis
- WBCs move from inside the blood vessel across the basement membrane. Basement membrane is rich in collagen IV and laminin. (Most common glycoprotein component of the basement membrane is Laminin).
- Facilitation of diapedesis is done by CD31/(PECAM)- platelet endothelial cell adhesion molecule.
Also Read: Acute inflammation: Symptoms, Causes, and Treatment : Pathology
Extravascular Change
- These changes begin when WBCs have crossed the vessel and they have a target to kill.
- Chemotaxis: It is defined as unidirectional movement of WBC to the site of infection.
- External chemotactic factors: Bacterial products.
- Endogenous chemotactic factors are C5a, IL8, LTB4.
- Targeted bacteria are then killed by process of “Phagocytosis”
- Components of Phagocytosis
- Opsonization: When WBCs come near bacteria they preferentially kill those bacteria which are coated by special chemicals named as opsonins, and this process is called opsonization.
- Chemicals required for opsonization are C3b, plasma proteins like fibrinogen, mannose binding lectin and immunoglobulins.
- Any condition in which there is hypogammaglobulinemia interferes with opsonization.
- Bruton’s Disease: Is X-linked recessive disease, hence mainly seen in boys.
- This condition is characterized by a B cell defect. There is a defect in enzyme B cell tyrosine signaling. As a result there is trouble in formation of antibodies and hence defective opsonization.
- Engulfment
- After opsonization of bacteria WBCs form pseudopod extension with the help of actin polymerization. Then WBC engulfs the bacteria. Now this trapped bacteria is present in the vacuole and is killed.
- Killing
- The bacteria in vacuole (phagosome) is brought near the lysosomes by the LYST (lysosomal transfer protein). Defect in LYST gene leads to Chediak Higashi Syndrome.
- Chediak Higashi Syndrome
- Features
- Absence of melanin pigment/ albinism.
- Recurrent infections.
- Presence of platelet defect (thrombocytopenia)
- Neurological manifestations
- Characteristic feature of chediak higashi syndrome is presence of GIANT granules in peripheral smear.
- Features
- KILLING can occur by 2 mechanisms
- Which do not use oxygen (O2 independent mechanism): This method involves use of proteins for killing the cell examples, arginine rich proteins, defensins, cathelicidin, eosinophilic basic proteins (EBP). EBP forms free radicals which are toxic specifically for parasites. EBP is also known as Major Basic Protein.
- Eosinophils are attracted to sites of inflammation by IL5, IL4.
- O2 dependent mechanism: This mechanism involves formation of free radicals and is much effective method of killing;
- Which do not use oxygen (O2 independent mechanism): This method involves use of proteins for killing the cell examples, arginine rich proteins, defensins, cathelicidin, eosinophilic basic proteins (EBP). EBP forms free radicals which are toxic specifically for parasites. EBP is also known as Major Basic Protein.
- Opsonization: When WBCs come near bacteria they preferentially kill those bacteria which are coated by special chemicals named as opsonins, and this process is called opsonization.
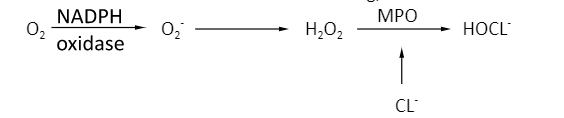
-
- (HOCL causes damage to infectious organisms). HOCL is also produced when bleaching powder comes in contact with water.
- Any defect in MPO results in increased risk of infections.
- NADPH oxidase is also given the name of respiratory burst oxidase.
- NADPH oxidase enzyme defect leads to chronic granulomatous disease (CGD) chronic granulomatous disease (CGD) - in this there is repeated attack of catalase positive organisms’ staph aureus and candida.
- Patients have granulomas in various organs of their body.
- Tests to be done: Dihydro rhodamine test, Nitroblue tetrazolium test (NBT)
- Management: Bone marrow transplantation, Interferon G.
Also Read: SICKLE CELL ANEMIA AND THALASSEMIA - NEET PG Pathology

Neutrophil Extracellular Traps
- Severe septicemia causes Platelet activation which activates an enzyme Arginine deaminase which converts arginine into citrulline. contents of neutrophils are excreted outside which forms a meshwork in which bacteria is trapped.
- This mechanism is activated at times of severe infection/sepsis. Neutrophil itself cannot survive afterwards.
- There is higher risk of development of systemic lupus erythematosus.
Emperipolesis
- In phagocytosis one cell engulfs another cell and engulfed cell dies but in emperipolesis engulfed cells are structurally normal and viable. No cell dies in emperipolesis.
- Seen in autoimmune hepatitis, Rosai Dorfman disease and also in myelodysplastic syndrome.
Entosis
- Cell within a cell phenomenon.
- These cells are in close contact with each other due to the presence of E- cadherin. In a tumor there is loss of E-cadherin and cells separate from each other and one cell engulfs the other cells.
- These cells are of the same type in contrast to emperipolesis where both cells are different and one bigger cell engulfs smaller cells.
- In entosis the dominant cell engulfs the weaker cell and the weaker cell dies. Entosis is seen in cancer cells where aggressive cells engulfs weaker cells to meet their energy requirements.
Also Read: CHRONIC INFLAMMATION: Symptoms, Causes, Diagnosis, and Treatment: Pathology
Chemical Mediators
Preformed Mediators
1. Histamine: Coming from mast cells. Stain for the mast cell is toluidine blue.
2. Serotonin
3. lysosomal enzymes
Newly Formed Mediators
- 1.Nitric oxide: It is a gaseous chemical mediator. Source of Nitric oxide is L-arginine.
- eNOS: Endothelial nitric oxide synthase
- iNOS: Inducible nitric oxide synthase
- nNOS: Present in nervous tissue
- 2.Cytokines
- Proinflammatory cytokines: IL-1, IL-6, TNFα. They contribute to systemic effects of inflammation. They are responsible for fever. (IL-18 is not associated with development of fever).
- Anti-inflammatory cytokines: IL-10, TGF-β, IL-11
- TGF-β is important in healing: It is a Profibrotic cytokine
- Dual acting: IL-4 and IL-6
- Interferons: INF
- α: It comes from lymphocytes
- β: It comes from fibroblasts
- γ: It comes from T-cells. It is responsible for macrophage activation, epithelial proliferation and plays a role in granuloma formation. It is used in management of chronic granulomatous disease.
- Chemokine
- α IL-8: It attracts the neutrophils
- β: Eotaxin, Rantes
- γ: Lymphotactin
- CX1c: Fractalkaline
- Cytokines act on the liver and cause an increase in concentration of certain proteins which are named as Acute Phase Reactants.
- Positive Acute Phase reactants
- Hepcidin: Involved in Pathogenesis of anemia of chronic disease
- Thrombopoietin
- Negative acute phase reactants
- Transferrin
- Albumin
- Transthyretin
- Positive Acute Phase reactants
Arachidonic Acid Metabolites
- Arachidonic acid is a 20-carbon fatty acid. Arachidonic acid is formed from phospholipase A2.
- Prostacyclin PGI2 causes vasodilation and anti-platelet aggregation.
- PGD2/E2/F2 causes fever and pain (mostly PGE2)
- Thromboxane A2: Vasoconstriction and platelet aggregation
- 5-lox(lipoxygenase): It is required for formation of 5-HPETE
- Leukotrienes: Leukotrienes C4/D4/E4/ are named as SRS-A (Slow reacting substance of anaphylaxis). Leukotrienes are involved in pathogenesis of bronchial asthma as they are very powerful bronchoconstrictor agents.
Inhibitors of arachidonic acid metabolites pathways
- PLA2 inhibitor: Corticosteroids.
- COX inhibitor: Aspirin, NSAIDS.
- 5 LOX inhibitor: Zileuton
- Leukotriene inhibitors: Montelukast zafirlukast
Kinin System
Factor 12 or Hageman factor causes
- Formation of kallikrein which forms bradykinin
- Activation of coagulation cascade
- Activation of fibrinolytic pathway
Bradykinin
- Actions
- Increased permeability
- Pain development
- Breaking of bradykinin is caused by ACE enzyme so patients on ACE inhibitors e.g. captopril, Ramipril there is increased bradykinin which is responsible for cough and angioedema.
Complement Pathway
- Complement pathway plays an important role in innate immunity as well as adaptive immunity.
- There are 3 pathways
- Classical pathway: In the classical pathway role is played by antigen and antibody. There is activation of complement proteins C4 and C2 which cause activation of C3. C3 cause activation of C5
- Lectin pathway: It starts with mannose binding lectin and there is formation of MAC (membrane attack complex). The formula of MAC is C5b-9.
- Alternate pathway: Alternate pathway is activated by gram negative infection, endotoxin exposure, IgA antibody
- Irrespective of initial pathway there is activation of MAC
- C3b helps in phagocytosis because it is involved in opsonization.
- C3a and C5a are involved in chemotaxis. They are anaphylatoxins
- Anaphylatoxins are involved in activation and degranulation of mast cells thereby causing release of histamine.
- C1 esterase inhibitor prevents excessive activation of the complement pathway. Deficiency of C1 Esterase Inhibitor causes Hereditary Angioneurotic oedema. It is a non-pitting type of oedema. (More commonly Females are affected, involves mucosal tissue like lips and tongue)
- Factor B/D or CD46: Its deficiency causes Atypical HUS (Haemolytic Uremic syndrome)
| Deficiency | Diseases |
| C1/C2/C4 | SLE |
| C3 | ↑ Pyogenic Infections |
| C5/ C6/ C7/ C8 | ↑ risk of infection by encapsulated organism (Meningococcus, Gonococcus as well as Toxoplasma |
- C2: Commonest complement deficiency reported in human beings
- CD55/CD59 deficiency causes PNH (Paroxysmal Nocturnal haemoglobinuria).
- C9 deficiency does not cause any disease.
Also Read: Cell Injury and Cell Dealth
Trisomy 18: Causes, Symptoms, Types, Diagnosis, Treatment and Prevention
Coagulation Cascade
- Thrombus formation has a TRIAD: Virchow’s triad
- Endothelial cell injury
- Hypercoagulability
- Altered blood flow / turbulence.
- Release of tissue factor causes activation of factor 7.
- Vitamin K dependent factors are 2,7,9,10. Out of these Factor 7 has the shortest half-life.
- Pregnancy is a hypercoagulable state. Majority of clotting factors are increased in pregnancy except Factor 11 which is decreased in pregnancy.
- Protein C and S inhibits factor 5 and 8 hence they are anticoagulant in nature
- For monitoring of extrinsic pathways, we use PT (Prothrombin time). Nowadays it is called INR.
- For monitoring of intrinsic pathways, we use ApTT (activated partial thromboplastin time).
- In Patient suffering from hemophilia there is increases in ApTT
- Patient suffering with chronic alcoholism or GI disease having steatorrhea having vitamin k deficiency will have increased INR
- For complete coagulation profile test done is thromboelastography (TEG)
- For performing PT and aPTT, use a plastic syringe (DO NOT take blood samples in a glass syringe because glass causes activation of intrinsic pathways).
- Perform the test within 2 hours of sample collection anticoagulant used is 3.2% trisodium citrate.
Also Read: Amyloidosis: Types, Causes, Symptoms, Diagnosis, Risk Factors, Treatment
We have more medical notes on high-yield topics for NEET PG Exam preparation, so stay tuned. Also, download the PrepLadder app and strengthen your exam preparation with high-quality study content and video lectures.
Download PrepLadder's NEET PG app for Android
Download PrepLadder's NEET PG app for iOS

PrepLadder Medical
Get access to all the essential resources required to ace your medical exam Preparation. Stay updated with the latest news and developments in the medical exam, improve your Medical Exam preparation, and turn your dreams into a reality!
Navigate Quickly
Overview
Types of inflammation
Acute inflammation
1. Vascular changes: Seen in Small vessels
2. Cellular changes
Intravascular
Leukocyte Adhesion deficiency disorders (LAD)
Extravascular Change
Neutrophil Extracellular Traps
Emperipolesis
Entosis
Chemical Mediators
Preformed Mediators
Newly Formed Mediators
Arachidonic Acid Metabolites
Inhibitors of arachidonic acid metabolites pathways
Kinin System
Bradykinin
Complement Pathway
Coagulation Cascade
Top searching words
The most popular search terms used by aspirants
- NEET PG Pathology
PrepLadder Version X for NEET PG
Avail 24-Hr Free Trial